The World Health Organisation has just published its status report on prison health in Europe. The report’s preface sets the context:
It is estimated that 6 million people are incarcerated every year in the WHO European Region. The prevalence of many health conditions is much greater among people in prison, who very often represent those “left behind”, compared with individuals in the community. Prison and other places of detention can provide an opportunity to deliver preventive and risk-reduction interventions and treatments to a population that previously may have had limited or no access to health care and healthy living.
It also summarises some sad, but not unexpected conclusions:
data from the Health in Prisons European Database (HIPED) paint a picture of an extremely vulnerable population that suffers from poor health and engages in risky health behaviours, leading to noncommunicable and communicable diseases and mental health conditions. Prevalence of indicators such as tobacco-smoking, injection drug use and
bloodborne viruses is shown to be much higher than generally is seen in the community. Furthermore, a large proportion of deaths in custody were found to be from suicide, which emphasizes the urgent need for Member States to safeguard the lives of individuals in their care by ensuring that prison health systems have appropriate screening and treatment for mental health disorders and suicide risk both on reception to prison and throughout an individual’s stay in custody.
Regular readers will be all too familiar with the shocking, and rising, number of suicides in English and Welsh prisons.
The report does not include individual country data nor comparisons between different states so I have sought merely to share findings that I hope are of interest to readers.
Prison staff and healthcare staff
On average, there are 209.6 prison staff and 31.7 health-care staff per 1000 people in prison. The ratio of different categories of health-care staff per 1000 incarcerated people is reported in the graphic reproduced below:
Prison environments
The WHO says that Prisons should be treated as a setting for health promotion and incarceration as a time during which individuals can address existing health conditions and improve lifestyle factors that may be contributing to their non-communicable disease (NCD) burden. The availability of a health-promoting environment, such as smoke-free cells, drug-free units and self-cook kitchen areas, is an important component of addressing NCD risk factors.
A tobacco-free environment encourages individuals to quit smoking tobacco (with appropriate nicotine replacement
therapy), while drug-free units encourage abstinence from illicit drug use and offer the opportunity to seek medical and psychological treatment. Self-cook kitchen areas promote better nutrition compared with traditional mass-produced prison meals and also contribute to individual autonomy and the development of skills in preparation for release from prison.
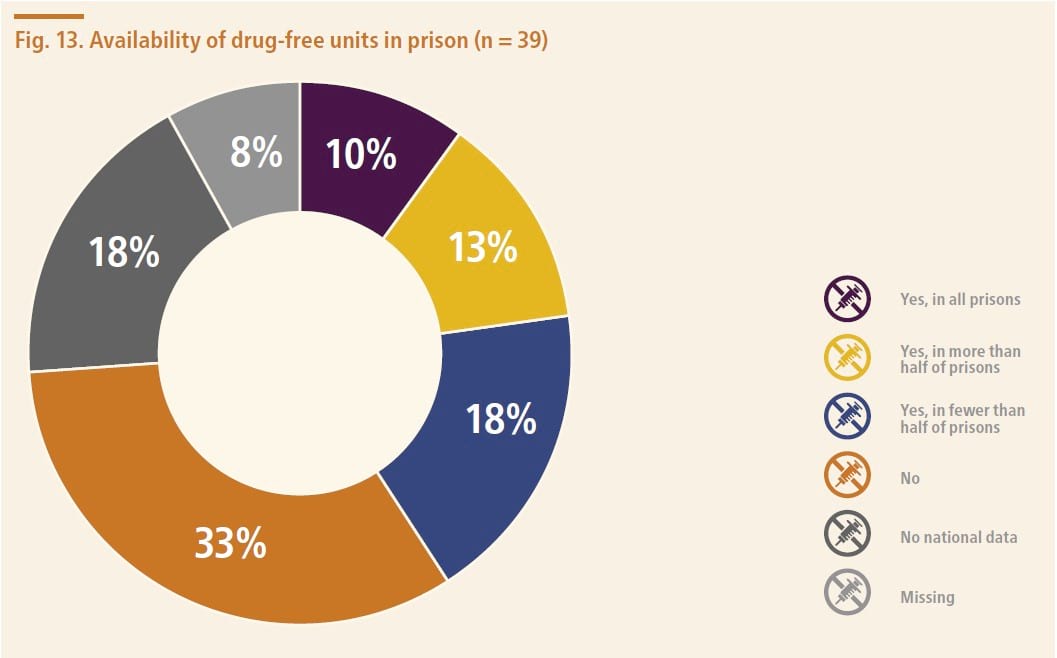
Drug-free units
Twenty-nine countries had national data available and provided a valid response regarding the availability of drug-free units in prisons. Among these countries, slightly more than half (55%) reported that drug-free units are available in prisons.
Substance use screening on reception
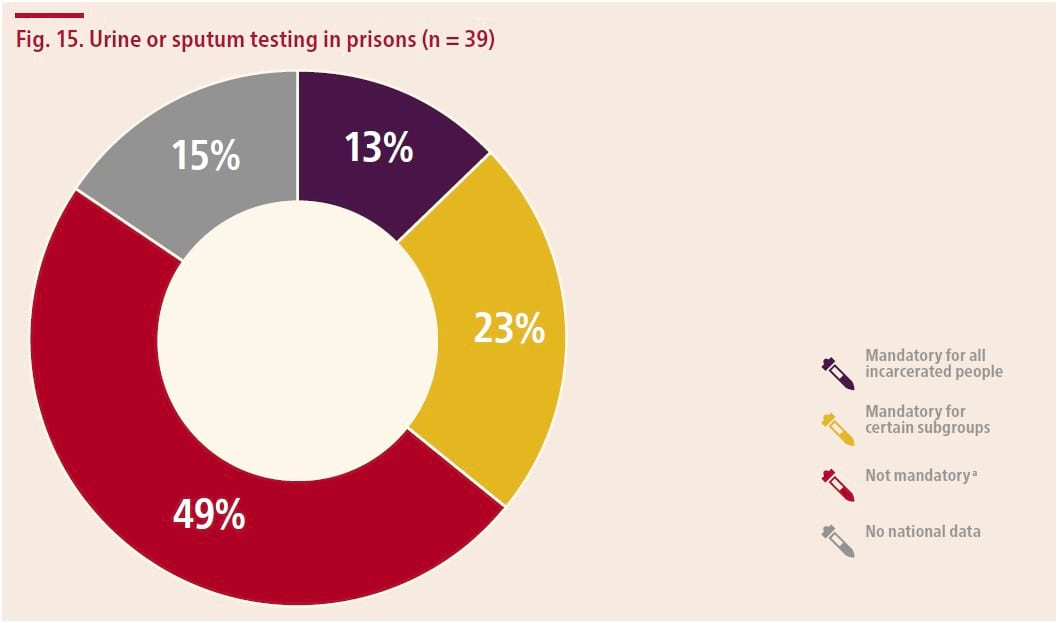
Urine or sputum testing requirements in prisons are presented in the graphic reproduced below. The subgroups for whom testing is mandatory included people with histories of drug use, people suspected of drug use and people receiving opioid maintenance therapy.
Of the 19 countries reporting that testing is not mandatory, 67% indicated that testing is available in prisons, 11% that it is not available, and 22% that other arrangements are in place (which include testing being used in some settings to confirm OST, and that it is used under the suspicion of substance use).
Few countries were able to provide national data on the prevalence of screening for illicit substance use and the prevalence of injecting drug use identified on reception to prison. The reported prevalence of current injection drug use based on responses from five Member States ranged from 5–26%, while the reported prevalence of lifetime injection drug use, also based on data from five (different) Member States, ranged from 0.72– 44%.
Of the 34 countries that provided data on the availability of screening for harmful alcohol use, 59% reported that it was implemented in prisons. Screening was implemented in all prisons in 80% of these countries. A validated screening tool was used to screen for harmful alcohol use in 47% of countries that provided data.
Screening for communicable diseases
Thirty-five Member States provided data on screening for HIV, 86% of which reported that HIV testing is available but not mandatory. Of the 36 Member States that provided data on screening for hepatitis B, 83% reported testing is available but not mandatory. Eighty-three per cent of the 35 Member States that provided data on screening for hepatitis C reported that testing is available but not mandatory. Of the 34 Member States that provided data on screening for STIs, 73% reported that screening for STIs is available on entry to prison.