The cost of tackling drug harms in prisons
Last Wednesday (4 February 2026), the National Audit Office (NAO) published a new report on “The Cost of Tackling Drug Harms in Prison”. The focus of the report is on how effectively the prison and health services are using public funds to tackle drug use within prisons, how funds are prioritised and how well the two services work together.
Increasing and rapidly changing threats
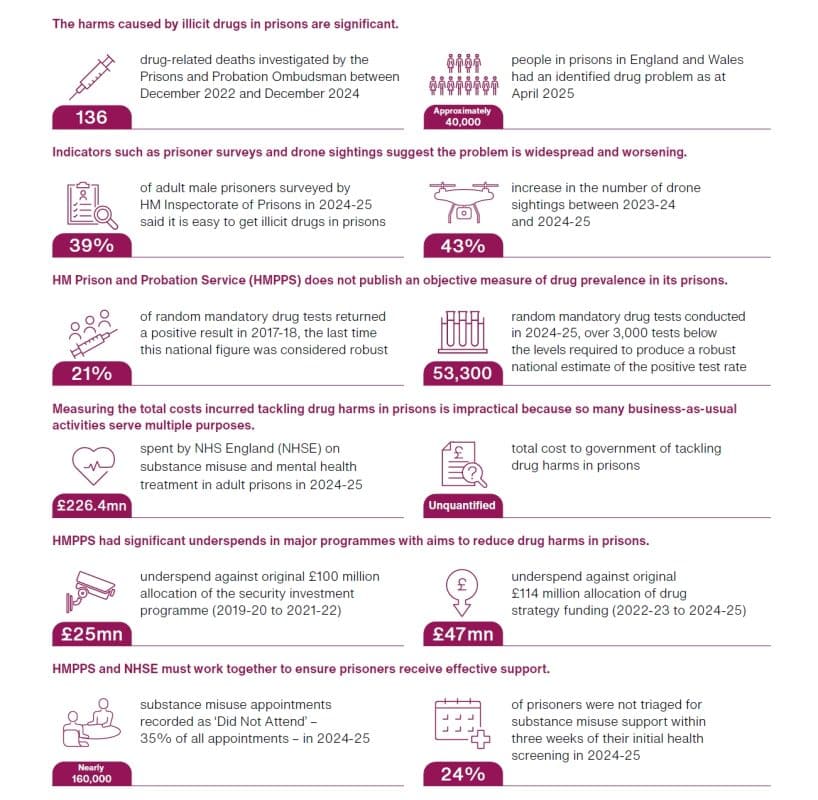
The prison and health services know that they face substantial, increasing and rapidly changing threats from illicit drugs in prisons. In 2024-25, HMPPS reported 26,348 drug find incidents, 25% more than the previous 12 months. The proportion of adult male prisoners reporting that it is easy to get illicit drugs in prison increased from 24% in 2021-22 to 39% in 2024-25. Two recent developments present growing threats: the availability of novel substances such as synthetic opioids has increased – these are more potent in smaller quantities than traditional drugs, harder to detect and easier to convey into prisons; secondly, criminals are increasingly using drones to convey drugs into prisons, with drone sightings increasing by more than 750% between 2019 and 2023 and by 43% between 2023-24 and 2024-25.
HMPPS needs to invest more
HMPPS has significantly underspent on two investment programmes that aim to reduce drug harms in prisons. Between 2019-20 and 2021-22, HMPPS spent only 75% of its £100 million security investment programme budget, with the largest underspend in gate security. HMPPS told us that the unspent funding was used to cover other operational activities. HMPPS was also allocated £114 million between 2022-23 and 2024-25 for prison-based and cross-cutting initiatives as part of the cross-government drug strategy From harm to hope. The actual budget was revised to £97 million to make savings and, of this, HMPPS spent only £67 million (69%).
And so does the NHS
NHSE spending on mental health and substance misuse treatment in prisons in England was lower in real terms in 2024-25 than it was in 2020-21. The combined spend on mental health and substance misuse treatment in prisons in England, not including primary care staff costs, was £226.4 million in 2024-25. Looking at the last five years, this represents a cash increase compared with the £202.9 million spent in 2020-21, but a real-terms decrease of 5%.
The use of resources
HMPPS has sought to reduce the quantity of drugs getting into prisons, but has been too slow in responding to urgent threats, leaving some prisons vulnerable. Prison governors said they do not have sufficient resources to respond to threats in an agile way. The NAO identified examples of broken security equipment not being repaired and work to improve window security taking several years.
The NAO is critical of the fact that Incentivised Substance Free Living (ISFL) wings or drug recovery wings have not been properly implemented and HMPPS does not know whether they represent good value for money.
Similarly, health commissioners have limited evidence to demonstrate that drug treatment services are improving or providing best value for money.
Partnership work
Capacity pressures and a lack of alignment between performance metrics for prison and health staff are hindering effective joint working. In February 2025, NHSE commissioners reported serious pressure on healthcare delivery in 35 prisons, of which 14 were “very likely to result in harm to patients”. In 2024-25, NHSE recorded nearly 160,000 substance misuse appointments as ‘Did Not Attend’ (DNA), around 35% of all appointments.
The NAO found that partnership working was weak with prison staff reporting they lacked the influence needed to improve health-related services, and NHS staff not always feeling sufficiently involved in decisions on prison operations and being reliant on prison staff to enable those services to be delivered safely.
Recommendations
The NAO makes five main recommendations:
- HMPPS should respond with more urgency to identified security weaknesses at specific prisons
- HMPPS and NHSE require better information on prevalence and need to prioritise funding
- Commissioners need better health needs assessments with a focus on substance use and standardised formulae to benchmark the cost of services and better KPIs
- Closer partnership arrangements which support better alignment of incentives to shared goals on health-related interventions
- HMPPS and NHS to draw on robust evaluation to understand what works and encourage best practice.
Thanks to Andy Aitchison for kind permission to use the header image in this post. You can see Andy’s work here