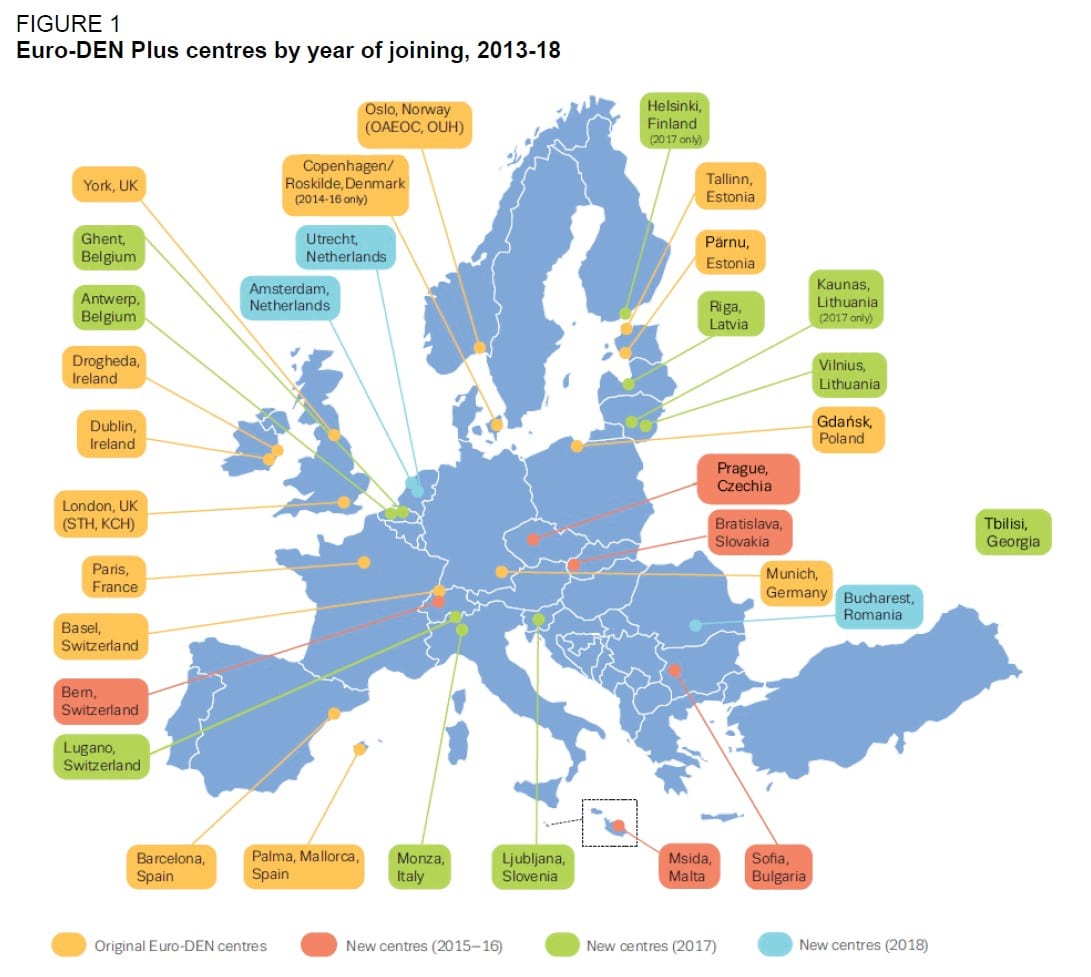
European data on hospital drug emergencies
The European Drug Emergencies Network (Euro-DEN) was established in October 2013 as a 2-year project funded by the European Commission Directorate-General for Justice, with the aim of improving knowledge at European level on acute established illicit/recreational drug and new psychoactive substance (NPS) toxicity
Euro-DEN Plus has expanded from the original 16 sentinel centres in 10 European countries in October 2013. In 2018, there were 31 active Euro-DEN Plus sentinel centres collecting data in 21 countries (Figure 1 below). There are three in the UK: King’s College Hospital, St Thomas’ & York.
Last week the European Monitoring Centre for Drugs and Drug Addiction published a report summarising the Euro-DEN Plus data for the 4-year period from 1 January 2014 to 31 December 2017 from 32 Euro-DEN Plus centres in 21 countries.
Main findings
Hospital emergency data can provide a unique insight into acute health harms related to drug use:
- There were 23 947 acute drug toxicity presentations reported by the Euro-DEN Plus centres over the 4-year period January 2014 to December 2017, representing a median of 0.3 % of all emergency presentations to the sentinel hospitals.
- More than 7 in 10 people presenting with acute drug toxicity arrived by ambulance, which has pre-hospital resource implications.
- Three quarters of those presenting were male, and presentations were most common among those aged 20-39 years.
- Three quarters of patients were discharged directly from the emergency department, and almost half were discharged within 4 hours. However, almost 1 in 5 of those discharged from the emergency department self-discharged, entailing lost opportunities for brief intervention, referral and care in the community.
- Although only a minority of patients were admitted to hospital, one quarter of those admitted required admission to the critical care unit because of severe clinical features.
- Opioids, and heroin in particular (the latter accounting for 22 % of all presentations), were the drugs most frequently encountered in acute drug toxicity presentations. Cocaine and cannabis were also prominent; these drugs were involved in 19 % and 17 % of presentations respectively.
- New psychoactive substances (NPS) were seen in 9 % of presentations over the 4-year period. There was significant geographical variation in the involvement of NPS in presentations, and the type of NPS that was predominant changed from cathinones in 2014-15 to synthetic cannabinoids in 2016-17.
- More than one quarter of all presentations involved the misuse of at least one prescription medicine, most commonly opioids and benzodiazepines such as methadone, diazepam and clonazepam.
- Presentations with acute drug toxicity constitute a significant burden on emergency health services; agitation and aggression are common features, and presentations are more common at weekends, in the late evening and at night.
Conclusions
Every year in Europe, thousands of individuals suffer drug-related acute toxicity that requires hospital attendance. These drug-related hospital emergency presentations are most likely to occur in young adults and to involve heroin, cocaine and cannabis. Findings from Euro-DEN Plus also highlight the potentially considerable burden on health services but also the potential for interventions. Over three quarters of cases are brought to the emergency department by ambulance and, while most cases are discharged quickly, a small but significant minority (6 %) involve severe acute toxicity requiring critical care admission, and some deaths are reported among this cohort. It is also important to note that clinical features associated with significant medical and nursing staff input, such as agitation/psychosis, are commonly seen in these patients. This has clear implications from a resource and staffing
perspective, particularly as these presentations are most common at weekends and in the late evening to early hours of the morning.
Data on hospital emergency department presentations provide a unique insight into acute health harms related to drug use, complementing data from the EMCDDA key indicators and broadening the scope of monitoring of the health consequences of drug use. This is particularly important in the light of the limited systematic data reported on acute drug toxicity in Europe. Findings from the Euro-DEN Plus project help to increase understanding of the drugs responsible for acute toxicity in Europe, whether they are illicit substances, NPS or misused prescription medicines. This dataset also enables analysis of geographical and time trends, patterns of acute toxicity and the potential implications of these presentations. The data do not necessarily provide a nationally representative picture, as only selected sites in participating countries are included. However, the increasing size and geographical reach of Euro-DEN Plus helps to minimise this limitation. Using a number of sentinel sites in significant locations provides useful data on the drugs resulting in presentations to emergency departments in Europe and the trends in these drugs and these locations over time.