Treatment population aging
Last week (3 November 2016) Public Health England published the drug and alcohol treatment stats for 2015/16.
It is clear from the data that there is an increasing need for services to meet the complex needs of older more vulnerable drug and alcohol users in treatment as well as finding ways of helping those accessing services for the first time to get the treatment they need and move on with their lives.
Heroin and alcohol only clients tend to be older than those in treatment because of their use of other drugs:

The figures
In all, 288,843 adults (aged 18 and over) were in contact with drug and alcohol services in 2015-16; which is a 2% reduction on the previous year.
Of these, 138,081 started their treatment during the year, with a large majority (97%) waiting three weeks or less to do so.
People with a dependency on opiates made up the largest proportion (52%, 149,807) in treatment in 2015-16. This is a fall of 2% compared to the previous year and a substantial reduction (12%) since the opioid treatment peak in 2009-10.
PHE remark that it is encouraging that the biggest fall in opioid treatment numbers is in younger adults, with a 79% reduction in people aged 18-24 starting treatment for opiate misuse since 2005-06.
Among the younger age group starting treatment, the majority reported problems with either cannabis (54%) or cocaine (24%).
Overall the number of under-25s accessing treatment has fallen by 37% since 2005-06, apparently reflecting the downward trend in drug use among younger people.
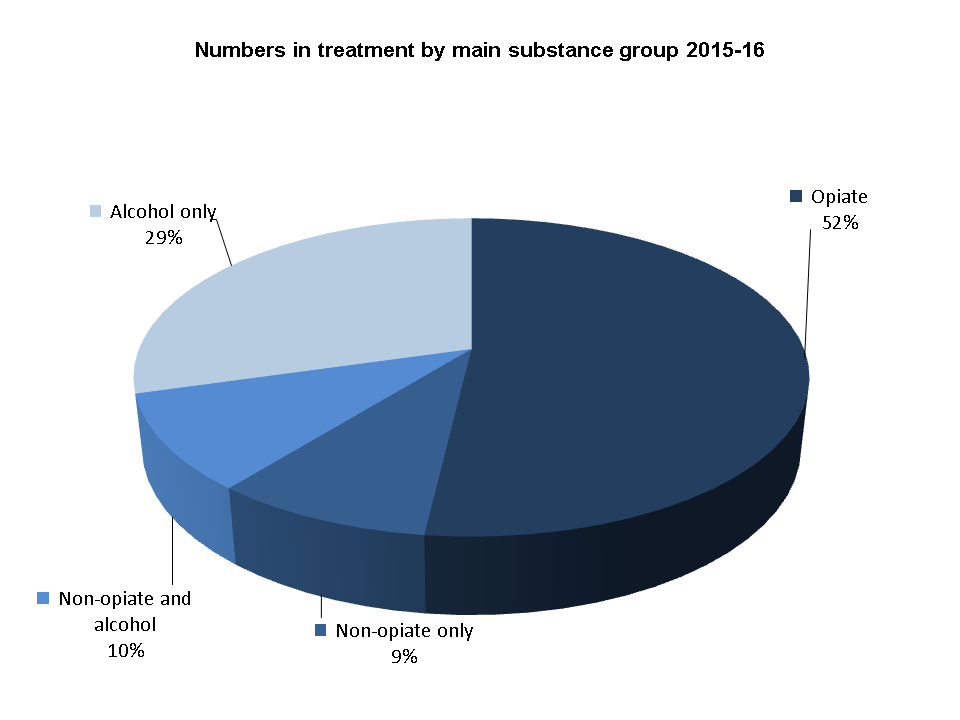
Those seeking treatment for alcohol made up the second largest group, with 144,908 people having problematic or dependent drinking.
Of these, 85,035 were treated for alcohol problems alone, and 59,873 for problems with both alcohol and other substances.
The overall number of people in treatment for alcohol fell by 4% compared to 2014-15, with the numbers in treatment for only alcohol decreasing by 5%.
Although the numbers are comparatively small (2,024), there was a 77% increase in people starting treatment for problems with new psychoactive substances (NPS), compared to the previous year.
This gives a clear signal to the treatment system of the need to be flexible and able to adapt to the differing needs of people accessing services.
While this sharp rise no doubt reflects increased use, PHE note that it may also partly reflect the bedding-in of new reporting categories to better capture NPS use.
The gender and ethnicity profile of those seeking treatment has changed very little over time, with the majority of people entering treatment in 2015-16 being male (70%) – men accounted for 73% in treatment for drug use and 61% receiving treatment for alcohol problems only.
White British still made up the largest ethnic group in treatment, at 85%.
Outcomes
In total, 127,080 people left the drug and alcohol treatment system in 2015-16, with 50% having successfully completed their treatment free of dependence. This compares to 52% last year.
Alcohol only clients had the highest rates of success on leaving with just under two thirds (62%) completing treatment successfully, up 1% on the previous year. This was followed by non-opiate only clients, with 60% leaving successfully, with a 4% decrease compared to 2014-15.
Opiate clients had the lowest rate of success in 2015-16 at 28%; this was down from 30% on the previous year and a peak of 37% in 2011-12. This lower success rate may reflect a large proportion of older opiate users now in treatment having entrenched long term drug use.
This group are often in ill health and are less likely to have the sorts of personal and social resources that we know can aid recovery, such as employment and stable housing.
Of course, these are not long-term outcomes with many individuals relapsing and returning for treatment in the future. The report provides some information on this issue; of the 154,471 individuals who were retained in treatment on the 31st March 2016, a third (31%) were in treatment continuously since their initial commencement. Just under a quarter (22%) were on their second treatment journey and 31% had more than three attempts at treatment:

Deaths
I have already covered the issue of drug-related deaths in some detail in previous posts but the increase has been of such magnitude over the last three years, that it is important to repeat the main figures here:
The number of people who died while in contact with treatment services in 2015-16 was 2,689 (0.9% of all individuals in treatment), this is an increase from 2014-15 when there were 2,360 deaths in treatment (0.8% of all individuals).
The number of opiate clients who died in treatment increased by 19% over the last year, (1,428 to 1,693) with deaths as a proportion of all opiate clients in treatment increasing from 0.9% to 1.1%. The median age of opiate clients recorded as having died in 2015-16 was 44 and 75% were male.
The number of deaths for users of other drugs increased from 140 in 2014-15 to 179 in 2015-16, an increase of 28%.
While not all deaths in treatment will be attributable to an individual’s substance use, the use of drugs is a significant cause of premature mortality in the UK. In England, the number of deaths from drug misuse registered in 2015 increased by 8.5% to 2,300, this follows an increase of 17% in the previous year and 21% the year before that.
The number of registered heroin deaths increased by 26% between 2014 and 2015 (953 to 1,201) and are now the highest on record. PHE makes the point that treatment has been shown to provide protection against drug related deaths and these numbers would likely be even higher without the harm reduction it provides.
Conclusion
It is difficult to conclude whether these figures are positive or not.
Does fewer people in treatment mean we should celebrate reduced demand?
Or are the figures more closely related to substantial cuts in treatment expenditure?
There are no reliable data on which to base a judgment either way.
Either way, the priorities clearly remain to improve the quality and effectiveness of treatment provided to long term opiate users and to stem the rise in drug-related deaths.








2 responses
Very useful article (I’m researching drugs and the elderly)
There was one item you quoted from PHE that I find confusing:
“In total, 127,080 people left the drug and alcohol treatment system in 2015-16, with 50% having successfully completed their treatment free of dependence. This compares to 52% last year.”
How can so many people be treated in the UK considering there are so few rehabs operational nowadays, and there doesn’t seem to be any NHS system to deal with alcohol and other addictions.
How do you account for this huge number? When i last checked the number of places in rehab clinics were in the hundreds
All the best
Rupert Wolfe Murray
Hi Rupert
Thanks for your comment.
Most of those people would have been attending community treatment agencies, not residential rehabs
Best Wishes
Russell