A changing world
The Global State of Harm Reduction 2016 has just (14 November 2016) been published. Produced by Harm Reduction International, this biennial report maps the response to drug-related HIV, viral hepatitis and tuberculosis.
It also updates information on harm reduction services in every region of the world, including on needle and syringe programmes (NSPs) and opioid substitution therapy (OST) provision; harm reduction services in prisons; access to antiretroviral therapy (ART) for people who inject drugs; overdose responses; policy developments; civil society developments; and information relating to funding for harm reduction.
With changing patterns in drug use, the 2016 report also reflects the use of, and harm reduction response to, amphetamine type stimulants (ATS).
Harm Reduction International
In 2008, Harm Reduction International (HRI) released the Global State of Harm Reduction, a report that mapped responses to drug-related HIV and hepatitis C epidemics around the world for the first time.
The data gathered for the report provided a critical baseline against which progress could be measured in terms of the international, regional and national recognition of harm reduction in policy and practice. Since then, the biennial report has become a key publication for researchers, policymakers, civil society organisations and advocates, mapping harm reduction policy adoption and programme implementation globally.
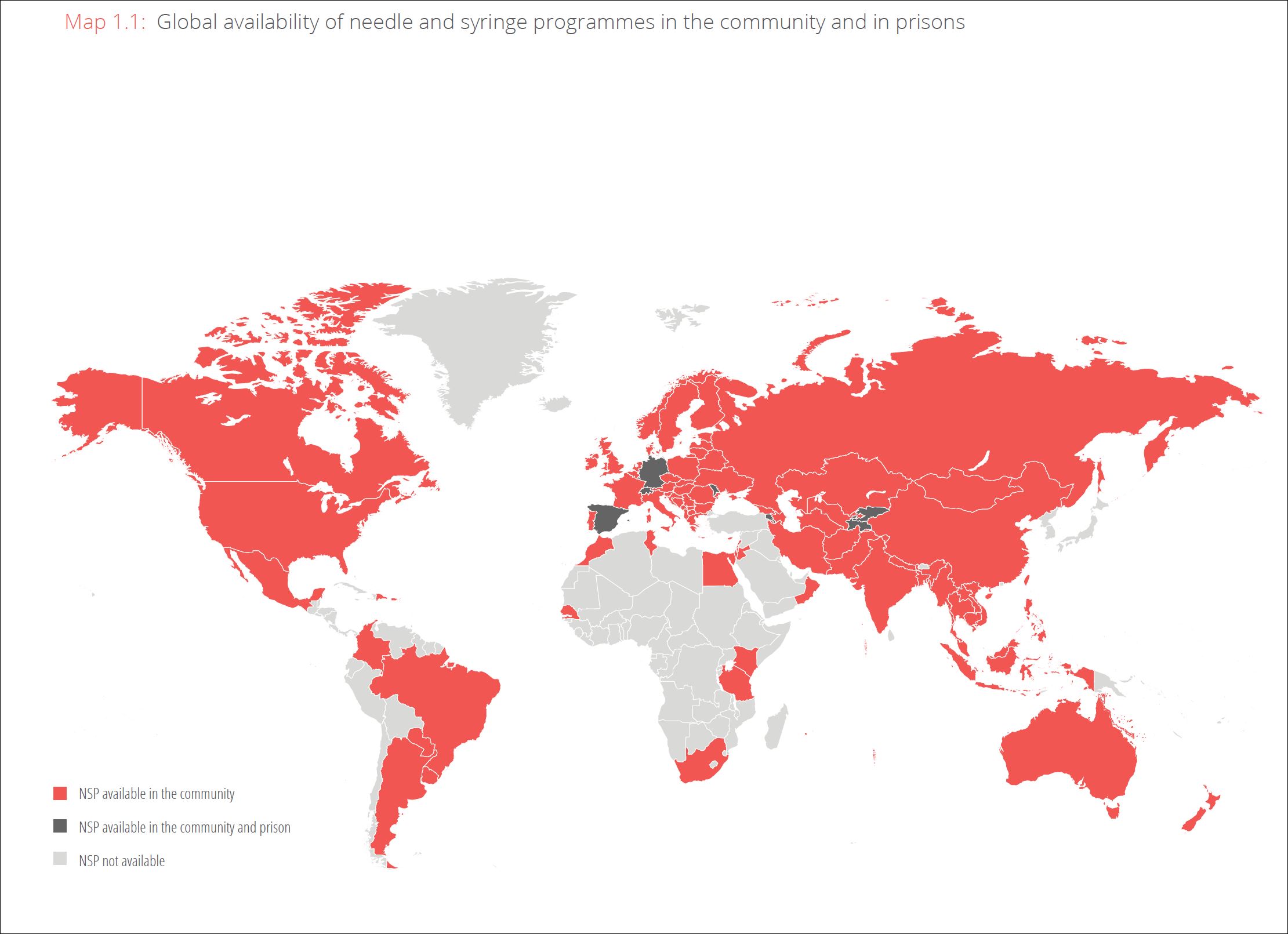
Since HRI first began reporting, the harm reduction response has increased globally with harm reduction programmes now operating at some level in more than half of the 158 countries in the world where injecting drug use has been documented. Harm reduction is now the majority response in the international community.
Global overview
Using primarily government reported data, UN estimates for 2014 found that 11.7 million people injected drugs worldwide, with 14% living with HIV, 52% living with hepatitis C and 9% living with hepatitis B. The harm reduction response, while in place to some degree in a majority of the world’s countries, falls far short of reaching most people who inject drugs worldwide.
In 2016, 90 countries implement needle and syringe programmes (NSPs) to some degree and 80 have at least one opioid substitution programme (OST) in place.
Perhaps the most striking statistic to emerge from this year’s Global State of Harm Reduction is that since 2014, there has been no increase in the number of countries implementing harm reduction programmes – the first time that this has happened since the inception of the Global State report in 2008.
Of 158 countries and territories where injecting drug use has been reported, 68 still have no NSP in place, and 78 have no provision of OST.

Western Europe
In much of Europe, HIV rates among people who inject drugs are reported to be stable or declining, with 1,236 newly reported drug-injection related HIV diagnoses in the European Union in 2014, the lowest number reported in more than a decade.
However, localised outbreaks of new HIV infections among people who inject drugs have been documented in Ireland, Scotland, and Luxembourg in 2015.
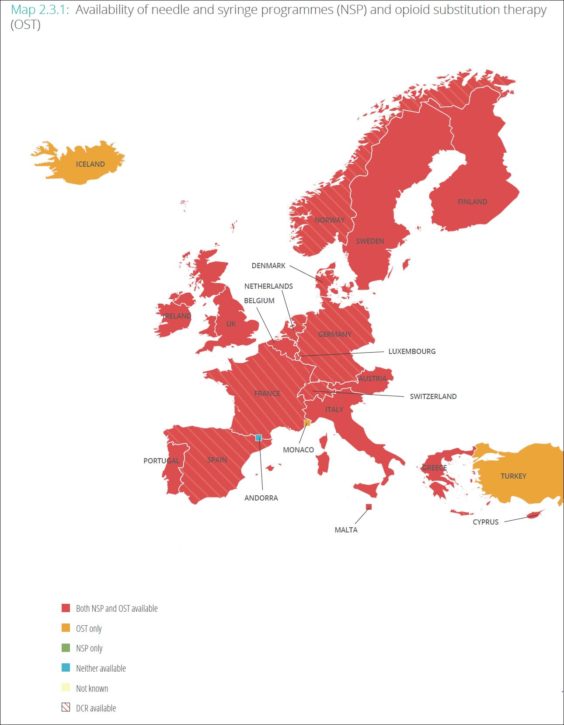
Although Western Europe is home to many of the strongest national harm reduction programmes in the world, with the vast majority of countries offering NSP provision and half of all opioid users accessing OST, there are still important gaps in service provision.
For example, access to hepatitis C treatment for people who inject drugs remains consistently low and new direct-acting antivirals (DAAs) continue to be priced out of reach. A myriad of factors, including criminalisation, stigma and inadequate medical and social services contribute to disproportionally high mortality and morbidity among people who use drugs in Europe, and overdose continues to be a major cause of death (which has increased sharply in the UK over the last three years).
There were an estimated 644,000 people who use opioids receiving OST in Western Europe in 2014, equating to about half of all people using opioids in the region. Coverage rates vary widely from low in Cyrpus, for example, to high in countries such as France and Portugal.
Methadone remains the most commonly prescribed form of opioid substitute, received by 61% of those receiving OST.
Drug consumption rooms
Alongside other effective harm reduction approaches such as OST and NSP provision, several countries in the region operate drug consumption rooms (DCRs).
These are professionally supervised healthcare facilities where people can consume drugs in safe conditions. The first supervised drug consumption room was opened in Berne, Switzerland in June 1986. In subsequent years further facilities were established in Germany, the Netherlands, Spain, Norway, Luxembourg, Denmark, Greece, and France.
Currently, there are 87 DCRs operating across eight countries in Western Europe: Denmark, Germany, Luxembourg, Netherlands, Norway, Spain, Switzerland and France.
In 2014, the only DCR available in Greece was closed due to policy makers’ failure to adpot the necessary legislative amendments. Both Norway and Luxembourg are preparing to open a second DCR but these may not be in operation until 2018. In January 2016, France approved a six-year trial of drug consumption rooms, with facilities opened in Paris in October 2016. Switzerland is also planning to open a further DCR in the near future, and Ireland is planning to introduce supervised injecting facilities during 2016.
There have been discussions about opening DCRs in various parts of the UK including Brighton & Glasgow but no firm plans to date.
Conclusion
The Global Review concludes by highlighting the need for continued funding of harm reduction in Europe:
There are concerns from civil society in many countries that the need for a well-funded harm reduction response is more pressing than ever, with drug use trends changing and NPS and stimulant use increasing. In order for harm reduction approaches in Western European countries to adapt to these new trends, adequate funds and political support is required.