Contingency management
Earlier this month (10 October 2016), the European Monitoring Centre for Drugs and Drug Abuse published a systematic review of the use of contingency management in drug and alcohol treatment.
“Contingency management” is the jargon for the sometimes controversial approach of using behavioural consequences to encourage drug users to stay in drug treatment or refrain from using illegal drugs. CM approaches, whereby rewards (e.g. cash, vouchers, prizes or other privileges such as therapy delivered at home) are contingent on successfully performing a particular activity (e.g. getting a job, providing a substance-negative urine sample, or participating in a screening) have been commonly used in the USA.
In the UK the National Institute for Health and Clinical Excellence (NICE) recommends that CM should be applied and assessed in routine clinical practice, identifying specific targets for application, such as increasing patients’ compliance with testing for infectious diseases.
The review
The review is based on analysis of 38 studies on opioid users (n = 20), cocaine users in methadone therapy (n = 14), cocaine users (n = 3) and methamphetamine users (n = 1) and 3 further papers about the cost-effectiveness of contingency management.
Contingency management can be used at different stages of the recovery journey:
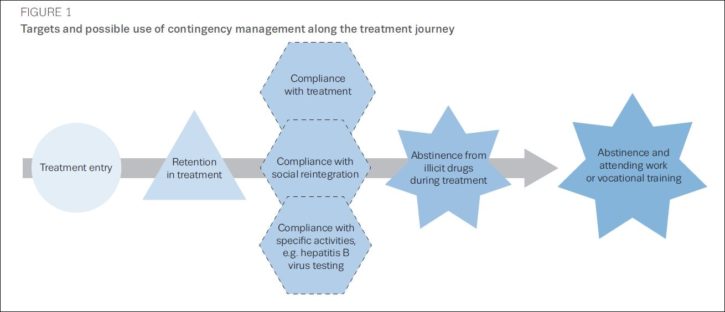
Results
The study found that contingency management has been shown to be effective with some treatment groups with some outcomes. The table below summarises the findings — where interventions are marked with a double plus (++), this means there was a positive effect on outcome in the majority of studies:
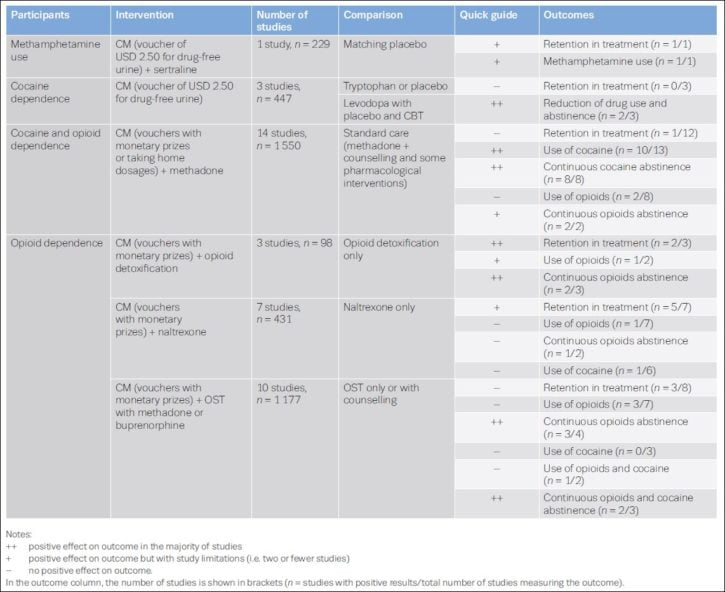
Contingency management is applied for a variety of interventions and settings and the overall results show that CM often helps to keep people in treatment, and it provides overall positive findings with opioid and cocaine addicts, but this is less clear for other substances.
Furthermore, the evidence seems to suggest that adding CM to other treatment approaches increases costs but can be a promising strategy overall if economic effects are considered.
The CM approach has been studied under very different conditions and settings. The participants enrolled in the studies which were analysed had problems related to stimulants, cocaine, opioids, and cocaine and opioids, or polysubstance problems. The CM approach was used as a stand-alone intervention, as an adjunct to other psychosocial interventions or in combination with pharmacological therapy.
Pharmacological treatments also varied, both in the objective (detoxification or maintenance) and in the type of drug used. Finally, CM approaches also varied, both in the types of behaviour reinforced (drug abstinence in the majority of studies, but also attending psychosocial therapy groups or compliance with the pharmacological treatment) and in the type of reward. Most of the trials used monetary rewards, but some used the possibility of taking home prescribed pharmaceuticals or the possibility of continuing to attend the therapeutic workplace.
Conclusion
The study authors acknowledge that the quality of the literature is variable. However, they conclude that:
Contingency management is a feasible and promising adjunct to treatment interventions for drug users.
Contingency management has been studied alongside various types of interventions provided in different settings. Overall, the study results show that CM can help keep people in treatment, and promote a reduction of opioid and cocaine problems in patients in opioid substitution treatment.
The provision of CM as an adjunct to other treatment approaches increases costs but, even though evidence is not yet strong enough to conclude on cost-effectiveness,the authors suggest that CM is a promising strategy overall provided the economic effects are considered in the long term.








2 responses
Hi there, thanks for the blog, v interesting! In the results table, can ‘-‘ refer to null effect and/or negative effect? Thanks
Hi Aisling
Thanks for your interest, I assume “_ ” can refer to either of those outcomes, the link to the document is in the blog post if you want to explore further.
Best Wishes
Russell