This is the fifth in a short series of posts on the RSA’s Future Prison project which sets out a blueprint for the modernisation of our prison system.
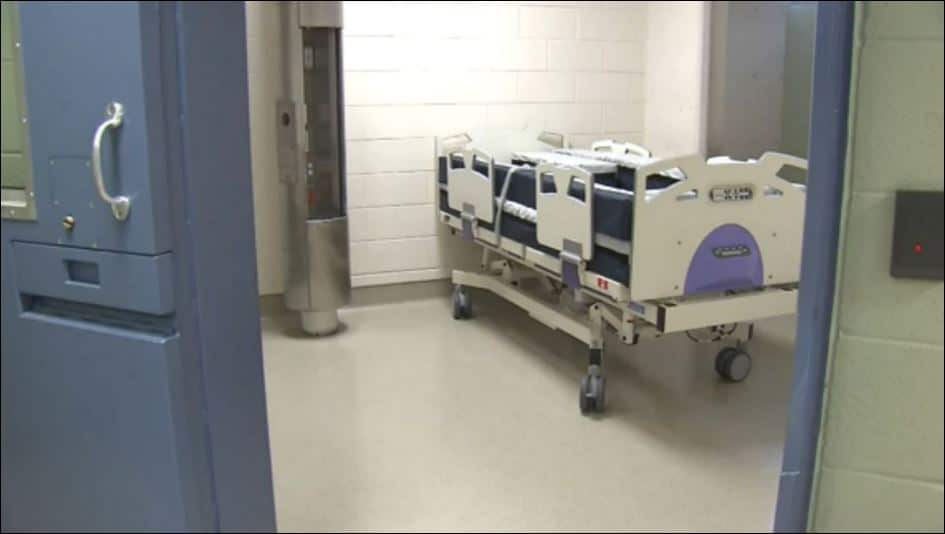
The state of prison healthcare
Prisons are not healthy places. Prisoners are more likely than the general population to have poor health before they come into custody, as well as poor diets, mental health problems and drug and alcohol issues.
This is particularly true of those who tend to return to prison again and again; for this reason, health provision available in both custodial settings and when people are released needs to be reconsidered – as does the relationship between the two.
In law, prisoners should be able to access the same health care as people living at home and should experience a seamless service when being released. However the commissioning arrangements which seek to achieve these goals are complex and in a state of flux following recent NHS reforms. Arrangements have also been further complicated and hampered by the recent changes to probation.
The growing levels of self-harm, surge in the use of legal highs inside and a rapidly ageing population are all big challenges for prison healthcare. These are aggravated further still by large cuts in staffing (down 30% in the last five years) and persistent over-crowding.
Mental health
Many of the most vulnerable in our society end up in prison. Our prisons are disproportionately filled with those who suffer from mental health issues with 25% of women and 15% of men reporting symptoms in line with psychosis – compared to just 4% in the general population.
Not only do people entering prison have far worse mental health than the general population, but there is significant evidence that prison can do more harm than good. Incarceration isolates people from family and friends, with detrimental impacts on mental health and well-being. Prisons can be violent and aggressive places with bullying and intimidation a real (and growing) problem in many establishments. We also put people in very unusual situations: a lack of freedom, cramped and unhygienic conditions in close proximity to people that they do not know can all contribute to a situation very damaging to mental health.
Fragmentation of commissioning
There is general agreement that, in spite of all its difficulties, moving health provisions the NHS as improved health services in prisons and few people would seek a return to the old Prison Health Service.
However, the NHS does not have a responsibility for reoffending which can lead to an inherent tension between managing the health service in a way that reduces problems for the prison regime and enhancing long-term rehabilitation. For example, there is good evidence that continuing prisoners’ methadone prescriptions during their sentence and ensuring continuity release reduce reoffending this presents considerable difficulties prison healthcare
a key challenge improving healthcare outcomes and increasing the chances of rehabilitation is how fragmented the commissioning of relevant services has become, both between prisons and the community and between different parts of the public sector.
The report summarises the complexity of current commissioning arrangements in the table below:
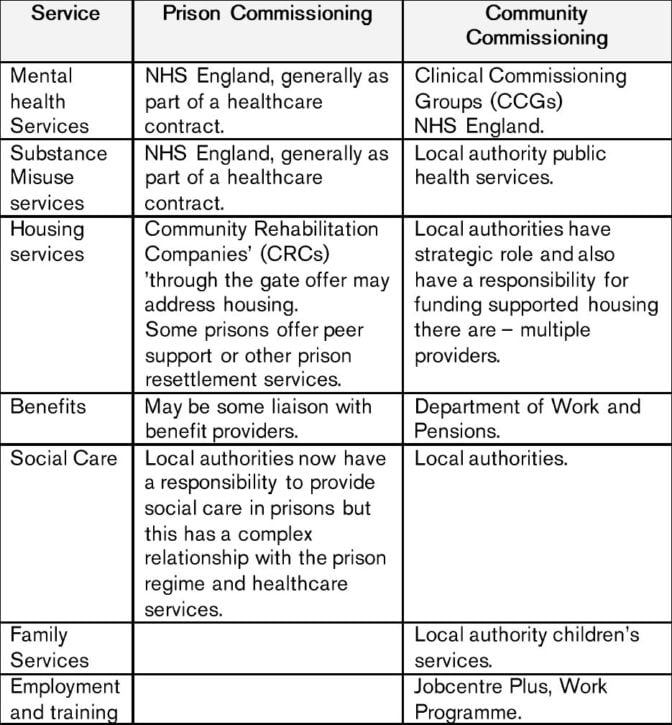
Prisons struggle to manage relations with a large number of different commissioners and providers for example, HMP Humber releases prisoners into Lincolnshire, Humber, York and North Yorkshire. This involves six unitary or upper tier authorities, five CCGs, one CRC, one division of the National Probation Service, a multitude of benefits offices, housing providers, NHS Trusts voluntary organisations and so on.
Constructing individual care plans to prisoners and then negotiating with this fragmented mosaic of community services across all these organisations is a formidable task.
Conclusion
The report sets out a number of key questions which the Future Prison will seek to answer over the next few months:
- How would a rehabilitative not-for-profit prison improve well-being inside and out?
- What are the current models of commissioning and what advantages and challenges do they bring?
- What institutional/cultural and individual barriers are there to supporting well-being and recovery; for example workforce skills and attitudes, competing demands et cetera?
- What is the experience of people leaving custody and in particular the role of the CRCs in relation to well-being services and drug, alcohol and mental health provision?
- What role could and should the liaison diversion arrangements bring?
- What role could and should a more sensible devolved set of responsibilities look like in relation to well-being – and can these build on the Care Act changes?